A tooth infection isn’t always obvious—but when left undiagnosed, it can quietly spread and cause serious health complications. So, how do dentists check for tooth infection? The answer lies in a step-by-step diagnostic process designed to identify the problem early and choose the safest, most effective treatment.
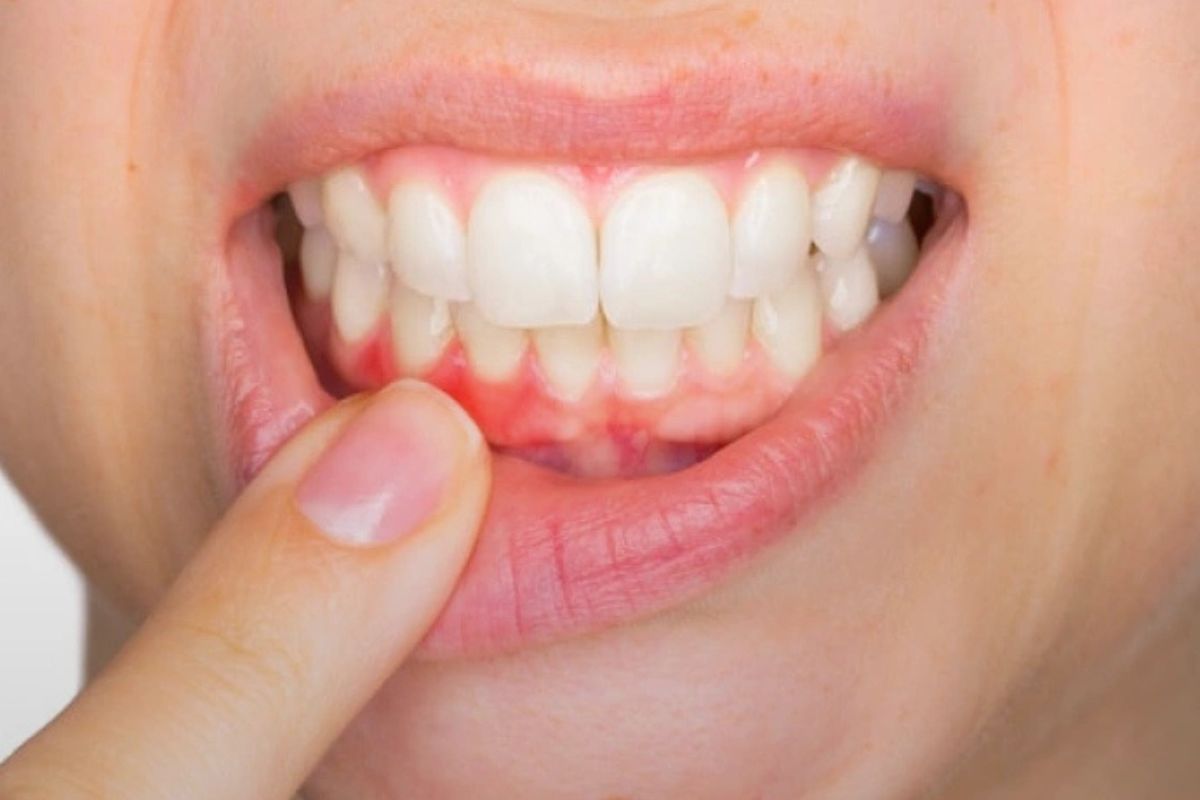
A tooth infection, often referred to as a dental abscess, occurs when bacteria invade the inner layers of a tooth or the surrounding gum tissue. Accurate diagnosis is critical—not just to relieve pain, but to prevent the infection from spreading to the jaw, sinuses, or bloodstream.
At Bartlesville Dental Studio, dentists focus on early, precise diagnosis to protect both oral and overall health.
What Is a Tooth Infection?
A dental infection begins when bacteria enter the tooth through decay, cracks, or gum disease. Once bacteria reach the pulp chamber, infection can build and form pus, leading to an abscessed tooth.
Common causes include:
- Untreated cavities
- Tooth trauma or fractures
- Advanced gum disease
- Failed dental restorations
Without treatment for gum disease, this can develop into a painful dental abscess.
Early Signs & Symptoms Patients Shouldn’t Ignore
Recognizing tooth infection symptoms early can prevent serious complications.
Common dental infection symptoms include:
- Persistent or throbbing tooth pain
- Sensitivity to hot or cold
- Swollen gums or face
- Bad taste or foul odor (abscess in mouth symptoms)
Red flags that require urgent care:
- Fever
- Swelling spreading to the cheek or jaw
- Difficulty swallowing or opening the mouth
These are advanced abscess symptoms that patients should never ignore.
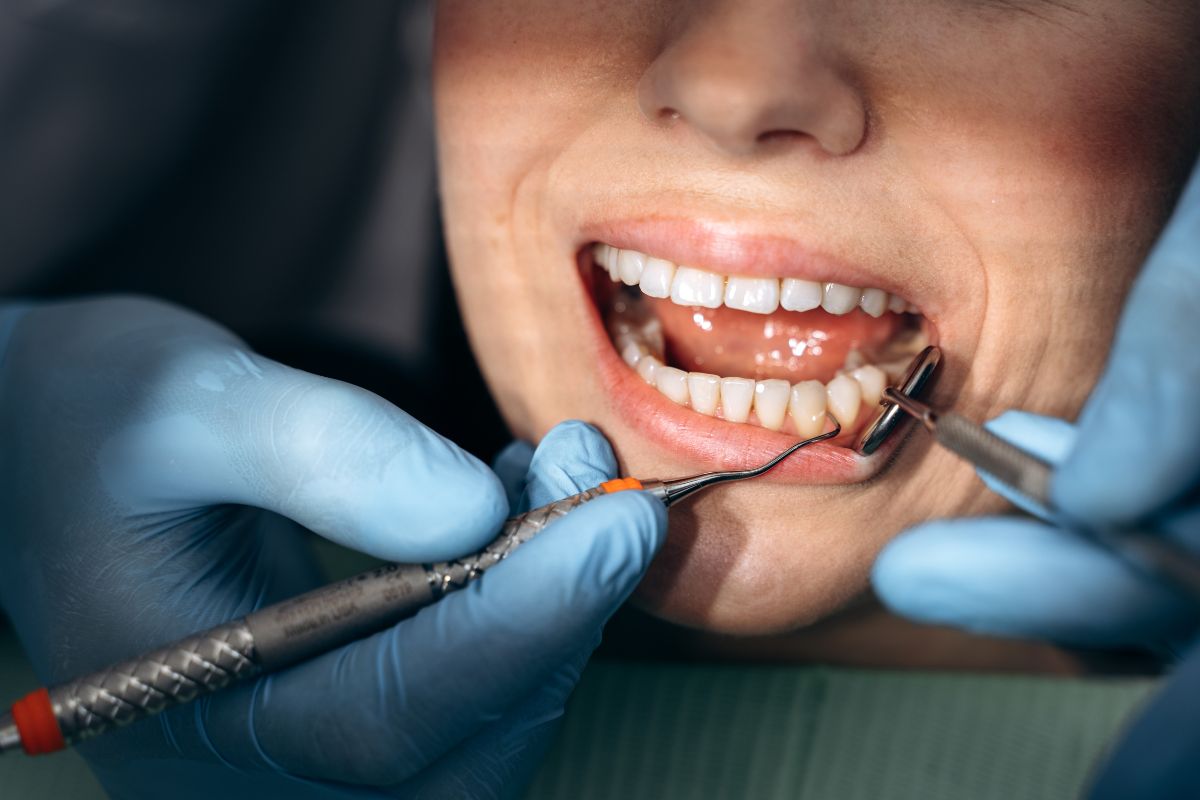
Initial Clinical Examination by a Dentist
Diagnosis begins with a thorough clinical exam.
Dentists assess:
- Gum color, swelling, or visible pus
- Tooth mobility or discoloration
- Tenderness around the tooth
- Nearby lymph nodes and tissue health
This exam helps determine whether a tooth abscess or deeper dental infection is present.
Dental X-Rays & Imaging
X-rays are essential for confirming infections that aren’t visible on the surface.
Dentists may use:
- Periapical X-rays to view the tooth root
- Panoramic X-rays to assess infection spread
- CBCT (3D imaging) for complex cases
Dentists look for dark areas near the root tip, bone loss, or hidden dental abscess pockets.
Functional Diagnostic Tests
To evaluate nerve health and inflammation, dentists use functional tests:
- Percussion test: tapping the tooth to detect inflammation
- Hot/cold sensitivity tests: assess pulp response
- Electric pulp testing: checks nerve vitality
Abnormal results often confirm tooth abscess symptoms or irreversible pulp damage.
Advanced Tools & Technology in Diagnosis
Modern dental technology allows for earlier and more accurate detection.
Dentists may use:
- Intraoral cameras for magnified, real-time visuals
- Digital scans for precise imaging
- Magnification loupes or microscopes
These tools help detect subtle dental infection symptoms before they worsen.
Related Assessments
Dentists also evaluate gum health through periodontal charting, which measures:
- Pocket depth
- Bleeding or infection around the tooth
This determines whether the infection is tooth-based or gum-related.
How Dentists Decide on Treatment
Once diagnosed, dentists choose the appropriate tooth abscess treatment based on severity.
Treatment options may include:
- Antibiotics (to control spreading infection)
- Root canal therapy to remove infected pulp
- Tooth extraction if the tooth cannot be saved
Complex cases may require referral to an endodontist for specialized dental infection treatment.
What Patients Should Do Before the Appointment
To help your dentist diagnose faster:
- Document symptoms, timing, and triggers
- List current medications
- Share recent dental work or trauma
Clear communication improves diagnostic accuracy.
Common Myths & Misconceptions
- “Every toothache means infection” — Not always; only a dentist can confirm.
- “Home remedies cure abscesses” — They may ease pain, but they won’t eliminate infection.
Professional care is essential for proper dental infection treatment.
Prevention Tips
Preventing a dental abscess starts with:
- Brushing and flossing daily
- Using fluoride toothpaste
- Regular dental exams and X-rays
- Treating cavities and gum disease early
Prevention reduces the risk of severe tooth infection symptoms.
Key Takeaway
So, how do dentists check for tooth infection? Through a comprehensive approach that includes clinical exams, imaging, diagnostic testing, and advanced technology. At Bartlesville Dental Studio, early diagnosis is key to stopping infection, relieving pain, and protecting long-term health.
If you notice abscess symptoms tooth or ongoing discomfort, prompt dental care can prevent serious complications. Book a consultation before it gets worse.
FAQs
Q. How long does it take a dentist to diagnose a tooth infection?
A: In most cases, a dentist can diagnose a tooth infection in a single visit using a clinical exam and dental X-rays.
Q. Can a dentist detect infection without X-rays?
A: Sometimes, visible signs are enough, but X-rays are usually needed to detect hidden dental abscesses.
Q. Will every tooth infection require a root canal?
A: No. Treatment depends on severity, and your dentist will recommend the most conservative dental infection treatment possible.
Q. How to get rid of a tooth abscess while pregnant?
A: See a dentist immediately. Professional treatment, such as drainage or a root canal, is essential, and pregnancy-safe antibiotics may be prescribed. Home remedies only offer temporary relief.
Q. Can a tooth infection cause fever?
A: Yes. A spreading tooth infection can cause fever, swelling, fatigue, and difficulty opening the mouth or swallowing, which requires urgent dental care.
Q. Can a tooth infection cause shoulder pain?
A: Yes. Referred nerve pain or muscle tension from a severe tooth infection can cause shoulder pain and may indicate the infection is spreading.
Q. How urgent is a tooth abscess?
A: A tooth abscess is a dental emergency. Seek immediate dental care, or go to the emergency room if you have a fever, facial swelling, or trouble breathing or swallowing.